Anesthesia
Anesthesia plays a critical role in the treatment and recovery of cancer patients at Moffitt Cancer Center. The Anesthesia Program is made up of a committed group of physicians, CRNAs, AAs and technicians dedicated to providing the best anesthesia care for our patients. While our primary focus is the safety of our patients in the operating room, we also provide patient care services outside of the operating room for a variety of medical and radiographic interventions.
-
Anesthesia and What to Expect
Prior to surgery, anesthesiologists evaluate the patient's medical condition and formulate an anesthetic plan for each individual patient, taking into consideration that patient's physical status. During surgery, advanced technology is used to monitor the body's functions. Anesthesiologists must interpret these sophisticated monitors in order to appropriately diagnose, regulate and treat the body's organ systems while a personalized, very delicate balance of anesthetic medications is administered. During recovery from anesthesia, pain control is tailored to each patient’s needs and clinical condition.
-
Preparing for Surgery
 Prior to your day of surgery, you will be in contact with our Pre-Anesthesia Testing (PAT) Clinic staff. One of our nurses will review your medical history and determine what type of visit would best fit your needs to ensure you are fully prepared for undergoing anesthesia. Using specific guidelines, our PAT staff will decide if you will need to come to the clinic to meet with our anesthesia advanced practice practitioner or if you can be seen virtually.
Prior to your day of surgery, you will be in contact with our Pre-Anesthesia Testing (PAT) Clinic staff. One of our nurses will review your medical history and determine what type of visit would best fit your needs to ensure you are fully prepared for undergoing anesthesia. Using specific guidelines, our PAT staff will decide if you will need to come to the clinic to meet with our anesthesia advanced practice practitioner or if you can be seen virtually.If you have a significant medical history, such as heart disease, diabetes or COPD, you will be asked to sign a release so we can obtain your records from your other doctors. In order to make sure it is safe to proceed with your scheduled surgery, you may also be asked to make an appointment with your other doctors so he/she may clear you for surgery at Moffitt.
-
Types of Anesthesia
- General Anesthesia
- A combination of medications to put you in a sleep-like state during surgery
- Mixture of inhaled and intravenous agents which produce amnesia (loss of memory), analgesia (loss of pain), and anesthesia (loss of consciousness)
- Usually requires a breathing tube which is placed after you are asleep and removed before you are awake.
- Anesthesia is very safe. The most common side effects are nausea/vomiting and sore throat from the breathing tube. Anything more than that is uncommon.
- Monitored Anesthesia Care/ Sedation
- Usually known as "twilight," this form of anesthesia renders you unconscious without the need for a breathing tube.
- Used for colonoscopy, endoscopy, procedures isolated to a small, peripheral portion of the body.
- Regional Anesthesia
- Regional anesthesia is a technique using local anesthetics (e.g. lidocaine) to numb a specific part of the body. It can be used as an adjunct to general anesthesia or monitored anesthesia care.
- Breast surgery (PECS block)
- Abdominal surgery (Epidural or TAP Block)
- Lower limb surgery (Epidural or Femoral/Sciatic)
- Upper limb surgery (Interscalene/Infraclavicular)
- Benefits of regional anesthesia
- Less narcotic and anesthesia is required for the procedure
- Better pain control
- Less nausea/vomiting
- Few opioid related side effects (constipation, grogginess, etc.)
- General Anesthesia
-
Regional Anesthesia
In addition to maintaining a decreased level of consciousness and awareness for patients undergoing surgical and select non-surgical procedures, anesthesiologists may use regional anesthesia in order to improve patient outcomes such as pain, nausea and vomiting and length of hospital stay.
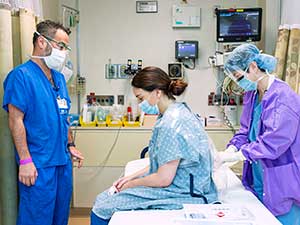
The specialty of regional anesthesia involves anesthetizing targeted areas of the body to decrease, and oftentimes eliminate, post-operative pain. Medical technology and innovation have enabled the development of multiple tools that anesthesiologists employ when performing regional anesthetics.
For instance, the use of ultrasound guidance and electrical nerve stimulation have dramatically improved the efficacy of peripheral nerve blockade and contributed to enhanced safety profiling as well.
As anesthesiologists, our goal is to provide improved surgical outcomes through interventions that minimize risk and are associated with a relatively low incidence of adverse effects.
With the intent of providing the best possible care available, we encourage our patients at Moffitt Cancer Center to engage in dialogue with their anesthesiologist regarding their candidacy for regional anesthetic techniques.
-
Patient Safety
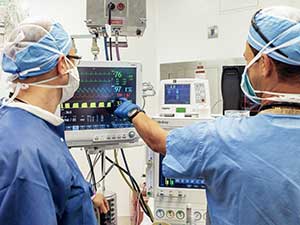 You’ll often hear or read an organization claim that "safety is our top priority." For the Moffitt Department of Anesthesiology, safety is not a priority, as priorities can be subject to change. For us, safety is the unwavering foundation upon which our practice of anesthesia is built.
You’ll often hear or read an organization claim that "safety is our top priority." For the Moffitt Department of Anesthesiology, safety is not a priority, as priorities can be subject to change. For us, safety is the unwavering foundation upon which our practice of anesthesia is built.Anesthesiologists have always been at the forefront of the patient safety movement. The Anesthesia Patient Safety Foundation (APSF) was the nation's first independent multidisciplinary organization created to help avoid patient harm and predated the National Patient Safety Foundation by more than a decade.
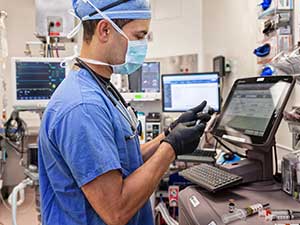 Moffitt Cancer Center anesthesiologists are proud to continue this legacy in patient safety. Our anesthesiologists have been the recipients of the Cancer Center’s Excellence in Safety Award three times, published articles on patient safety, and have been invited to share their expertise at international meetings.
Moffitt Cancer Center anesthesiologists are proud to continue this legacy in patient safety. Our anesthesiologists have been the recipients of the Cancer Center’s Excellence in Safety Award three times, published articles on patient safety, and have been invited to share their expertise at international meetings.Through the use of surgical safety checklists, a systems-based approach, and teamwork, we are dedicated to getting you safely through surgery.
Preparing For Your Surgery
