What is Melanoma?
A type of skin cancer, malignant melanoma forms in skin cells called melanocytes, which produce the pigment that gives the skin its color. Known as melanin, this pigment also helps protect the deep layers of skin from the harmful effects of ultraviolet (UV) light exposure.
Healthy melanocytes and other skin cells normally develop in a controlled and orderly fashion. As new cells form, they push older cells toward the surface of the skin, where the old cells eventually die and flake off. Like all cancers, malignant melanoma results from abnormal cellular DNA changes that cause the cells to grow uncontrollably. The excess cancer cells then build up, bind together and form tumors.
How common is melanoma?
In the United States, melanoma is the fifth most commonly diagnosed cancer among both men and women. The number of new cases diagnosed each year has increased steadily for the past 30 years.
Skin carcinoma vs. melanoma
Melanoma is far less common than non-melanoma skin cancer, such as basal cell carcinoma or squamous cell carcinoma. However, melanoma is generally more serious because it is more likely to grow and spread to other areas of the body.
Signs of melanoma
Although melanoma skin cancer can develop virtually anywhere on the body, it is most often found in areas that are exposed to the sun, such as the face, back, arms and legs. The first noticeable symptom may be:
- A change in an existing mole
- A new skin growth
An atypical mole vs. melanoma
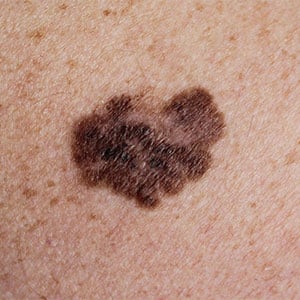
A normal mole can be tan, brown or black. Generally, the color will be uniform, and there will be a distinct border between the mole and the surrounding skin. Most noncancerous moles are round and smaller than 6mm in diameter, which is about the size of a pencil eraser.
For general awareness purposes, a commonly used melanoma definition is an unusual mole that has one or more of these “ABCDE” characteristics:
- Asymmetry – Two very different-looking halves
- Border – An undefined, scalloped or notched border
- Color – Several colors or one non-uniform color
- Diameter – Larger than 6 mm across
- Evolving – Changes in size, shape or color over time
Melanoma is sometimes misdiagnosed as seborrheic keratosis. Despite the similar appearance of the lesions, however, there is a key difference between seborrheic keratosis vs. melanoma. Specifically, seborrheic keratoses are harmless growths that often develop as a consequence of the aging process—and are benign. Melanoma, by definition, is malignant.
What causes melanoma?
The precise causes of the cellular DNA changes that lead to the development of melanoma skin cancer are not yet fully understood by scientists in the general medical community. However, researchers have conclusively established that exposure to UV light from the sun and other sources, such as tanning beds, greatly increases the risk of melanoma. As such, according to the American Academy of Dermatology and the Skin Cancer Foundation, the best way to avoid developing melanoma cancer is to stay out of the sun.
Even so, not all melanomas result from UV light exposure. Some melanomas, which are often referred to as hidden melanomas, develop in areas of the body that are never exposed to the sun, such as:
- Under a fingernail or toenail (the lesion may resemble a subungual hematoma, which is a pooling of blood in the nail bed that may develop within a few days of a crushing injury; however, the main difference between a subungual hematoma vs. melanoma is that the nail discoloration from the former will gradually clear up as the nail heals)
- Between two fingers or two toes
- On the palm of a hand or the sole of a foot
- Under the hair on the scalp
- Inside the nose, mouth or digestive tract
- On the genitals
- Inside the anus, vagina or urinary tract
For this reason, many experts believe melanoma cancer occurs due to a combination of genetic and environmental factors.
In addition to UV light exposure, other risk factors for melanoma skin cancer include:
- Fair skin
- A history of sunburn
- More than 50 moles (most adults have between 10 and 40 moles)
- A family history of melanoma
- A weakened immune system
Although melanoma on black skin tends to occur less frequently than melanoma on white skin, it is important to note that people of all colors, including those with black and dark brown skin, can and do get skin cancer.
Types of melanoma
The most common type of melanoma cancer is skin (cutaneous) melanoma. Cutaneous melanoma usually begins in the top layer of the skin (epidermis). If left untreated, it can potentially spread and invade the deeper layers of skin, such as the dermis and hypodermis.
The subtypes of cutaneous melanoma include:
- Superficial spreading melanoma
- Nodular melanoma
- Lentigo maligna melanoma
- Acral legtiginous melanoma
- Desmoplastic melanoma
- Amelanotic melanoma
Less common than skin melanoma, the other types of melanoma cancer are:
- Ocular melanoma – Develops in an eye
- Mucosal melanoma – Develops in a mucous membrane, such as the lining of the nose, mouth or digestive tract
- Melanoma with an unknown primary (MUP) – Spreads within the body from a tumor of unknown origin
- Pediatric melanoma – Any melanoma that develops in a child
How is melanoma treated?
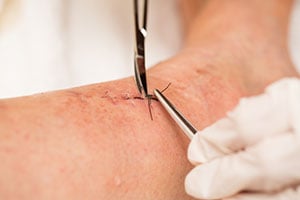 Melanoma treatment can vary depending on the extent of the cancer and the patient’s overall health and preferences. In many cases, early-stage melanoma skin cancer is treated with surgery. Sometimes, an entire melanoma can be removed during a biopsy and no further treatment is necessary.
Melanoma treatment can vary depending on the extent of the cancer and the patient’s overall health and preferences. In many cases, early-stage melanoma skin cancer is treated with surgery. Sometimes, an entire melanoma can be removed during a biopsy and no further treatment is necessary.
The treatment options for metastatic melanoma, which has spread beyond the skin, may include:
- Surgery – Removal of the malignant melanoma and any affected lymph nodes (as identified through a sentinel lymph node biopsy.)
- Immunotherapy – Medication that helps the body’s immune system identify and eliminate the cancer. A first-of-its-kind immunotherapy pioneered at Moffitt called TIL therapy takes advantage of the immune system’s ability to seek out and fight cancer cells.
- Targeted therapy – Medication that destroys the melanoma by targeting its unique cellular characteristics.
- Radiation therapy – High-energy beams, such as X-rays or protons, that target and kill melanoma cells.
- Chemotherapy – Medications (administered orally or intravenously) that travel throughout the body to find and destroy cancer cells.
What is the melanoma survival rate?
Usually, the melanoma cancer survival rate is discussed within the context of a five-year timeframe. Research studies completed over the last decade show a significant rise in the overall five-year survival rate of patients who develop malignant melanoma. Some experts attribute this trend to improved education and awareness of the importance of skin cancer prevention. Other key factors include better diagnostic techniques, which allow more tumors to be detected when still confined to a shallow skin depth, and advances in surgical techniques and other treatments such as immunotherapy and targeted therapy.
Although the melanoma survival rate is accurate for a certain group of people, it does not provide a complete picture for any one individual. Also, the data used to calculate it is highly complex and based on the experiences of patients who were treated at least five years ago when many of today’s advanced treatments were not yet available. On the whole, however, the prognosis for melanoma patients is continually improving.


Top 1% of Cancer Hospitals
Schedule an AppointmentOur melanoma treatment approach
The multispecialty team in the Cutaneous Oncology Program at Moffitt Cancer Center specializes in the diagnosis and treatment of melanoma and all other forms of skin cancer. In one convenient location, our patients can benefit from the latest options in skin cancer screening, diagnosis, staging, treatment, supportive care and long-term follow-up. To ensure the best possible care, we create an individualized treatment plan for each patient. Complex cases are reviewed by our tumor board of skin cancer specialists, which includes:
- Surgeons
- Medical oncologists
- Dermatologists
- Dermatopathologists
- Radiologists
- Radiation oncologists
- Plastic surgeons
- Registered nurses
Melanoma cancer research is a primary focus of the Moffitt team. The scientists in our renowned Melanoma and Skin Cancer Research Center of Excellence work together to better define melanoma, enhance our understanding of skin cancer and quickly bring new laboratory developments to clinical trials. We are proud to be the only National Cancer Institute-designated Comprehensive Cancer Center based in Florida, which is a testament to our dedicated research efforts. Through our groundbreaking discoveries, we continue to improve survival rates and enhance the quality of life for current and future melanoma patients.
If you would like to request an appointment with a skin melanoma specialist at Moffitt Cancer Center, call 1-888-663-3488, or complete a new patient registration form online. We will connect you with an expert as soon as possible, who will further explain the melanoma definition and answer any questions you may have about basal cell carcinoma vs. melanoma.
Learn more about the Melanoma Research Center of Excellence



