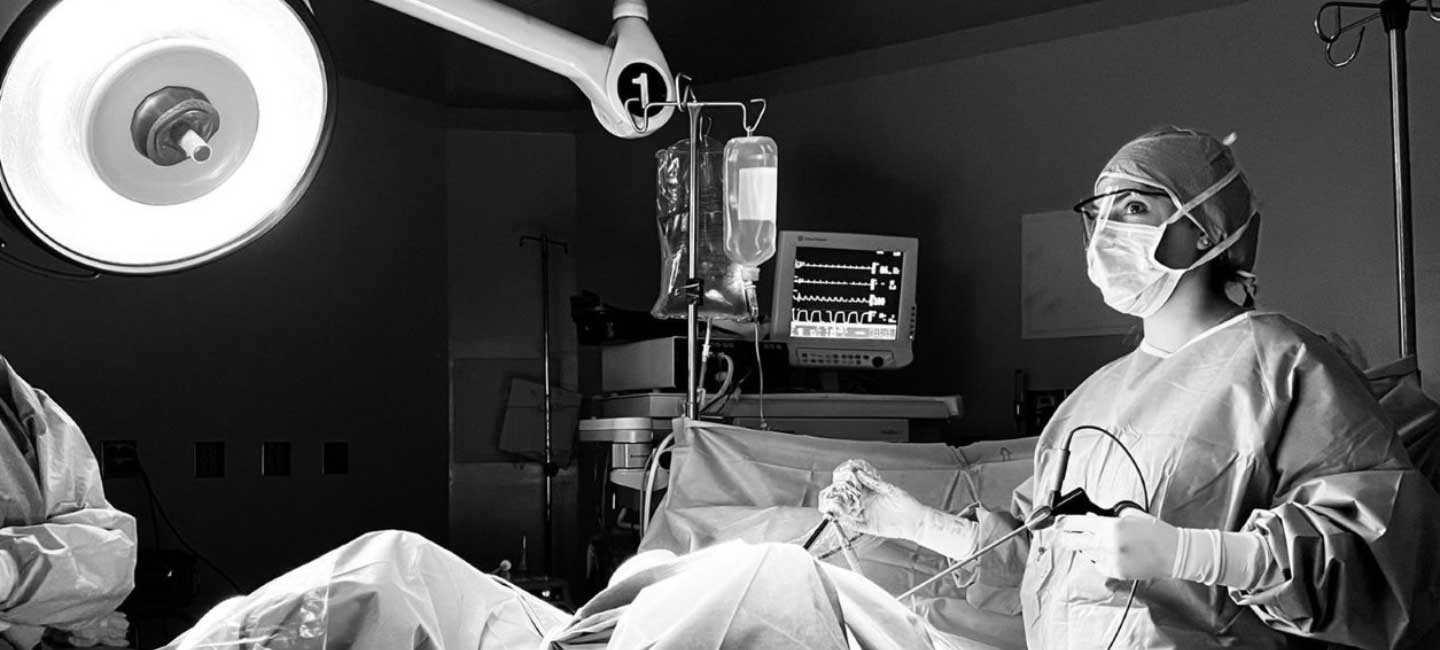
Moffitt Doctor Brings Cervical Cancer Care to Central America
It’s estimated that nearly 14,000 women will be diagnosed with cervical cancer in the United States this year. According to the American Cancer Society, about 4,310 women will die from the disease. Cervical cancer used to be one of the deadliest forms of cancer for American women, but thanks to the developments of HPV and Pap testing, mortality rates have steadily fallen.
Outside of the United States, however, the numbers aren’t as promising. Cervical cancer is the fourth most diagnosed cancer in women worldwide, with 85% of cases in low- and middle-income countries, according to a 2010 study.
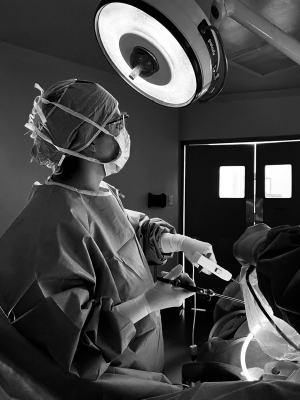
Dr. Monica Avila operates on a patient in Guatemala (Photo by Amy Blok).
In Guatemala, an estimated 1,555 women are diagnosed with cervical cancer each year. More than half will die.
Dr. Monica Avila is trying to change that.
Avila, an oncologist in the Gynecologic Oncology Program at Moffitt Cancer Center, began what she plans to be an annual medical mission trip to Guatemala to bring her North American health care knowledge to the Central American country.
“It’s hard because it’s such a resource limited area,” Avila said. “It’s not your traditional model where you have access to CT scans, MRIs or PET scans. So you have to get creative and use your clinical gut to be able to diagnose some of these diseases. Even having access to a pathologist that diagnoses the cervical cancer is really hard to come by. We’re typically only allowed to send off a very high-risk specimen that you have a very high suspicion for cancer.”
Avila made her first trip to Guatemala last year with a group of surgeons and nurses. She was inspired to bring her expertise worldwide after visiting Peru during her medical school training. It was there where she would screen women for cervical cancer who in some cases had walked hundreds of miles seeking treatment.

Dr. Monica Avila, gynecologic oncologist
During her visit to Guatemala, Avila and her colleagues set up a fully functional operating room. Without access to many of the diagnostic equipment available in the U.S., surgery was often the only treatment option. One of the surgeries Avila typically performed was radical hysterectomy to remove a patient’s uterus, cervix and surrounding tissue.
“The thought is that that is where cervical cancer really spreads geographically side to side,” Avila said. “So that would be the first place where it would invade. If we clear that parametrial tissue, then hopefully we’ve cleared all the disease.”
While Avila will travel to Guatemala annually, her care will continue on a monthly basis as part of Project ECHO, a digital health care approach started by the University of New Mexico for sharing knowledge in rural and underserved communities around the world.
“It’s so critical because we have the tools, even with surgery alone, to cure somebody of cancer,” Avila said. “To watch somebody die of a preventable and curable disease is just heartbreaking. The reason that I do it is just knowing that I may potentially be able to cure somebody.”