Sentinel Lymph Node Mapping for Uterine Cancer
Endometrial cancer begins in the lining of the uterus and is sometimes called uterine cancer. It is often detected at an early stage because it causes irregular bleeding and pelvic pain.
Historically, surgeons relied on lymphadenectomy to identify the presence of endometrial cancer cells. However, the innovative gynecologic oncologists at Moffitt Cancer Center are performing sentinel lymph node (SLN) mapping as a less-invasive alternative. Learn more about our standard of care and what the future looks like for uterine cancer treatment.
Lymph Node Evaluation is the Standard of Care For Uterine Cancer
The practice for identifying cancerous endometrial cells is a lymphadenectomy, also known as a lymph node dissection or removal. This practice lets the doctor understand the exact stage the cancer is in while potentially slowing the spread of the disease through the removal of cancerous cells.
The lymphadenectomy is performed through an incision in the abdomen while the patient is under general anesthesia. A lymphadenectomy is often recommended if the surgeon has seen existing cancer cells and wants to understand how far they have spread.
While lymphadenectomy is an effective way to identify the prevalence of cancer cells, it comes with its own risks. Patients still need to undergo surgery and have the strength to recover afterward. In some cases, this operation can lead to further complications related to cancer, creating a harder fight for patients.
How Sentinel Lymph Node (SLN) Mapping Works
Moffitt Cancer Center is always looking for better ways to treat patients. They want to catch the presence of cancer cells earlier and use less invasive methods to treat the disease. Therefore, more surgeons are turning to SLN mapping.
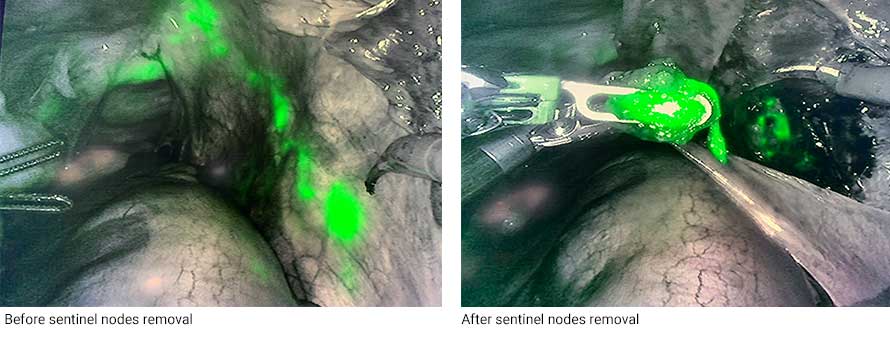
With this option, surgeons use blue or green dye with immunofluorescence to highlight the lymph node. Essentially, the lymph nodes light up with a neon glow that makes them easier to see. The cervix is injected with a dye that travels up to the lymph node chain. Not only is this an effective technique for mapping pelvic lymph nodes, but there are some occasions when SLN mapping will also provide a clear view of lower aortic nodes.
Benefits of SLN Mapping
"There are several benefits of SLN mapping for both surgeons and patients. The first benefit is the less-invasive nature of the procedure. SLN mapping is done at the time of surgery to remove just the lymph node. As a result, the patient doesn't have to undergo full lymph node dissection thus reducing the risk of potential infections, leg swelling called lymphedema, blood clots, or potential injury to nearby blood vessels, nerves, or nearby organs," said Dr. Monica Avila, a gynecologic oncologist in the Department of Gynecologic Oncology.
Another reason to consider SLN mapping is that it's not new to the world of cancer. This form of mapping is used in other cancer types and is only new to the identification of endometrial cancer cells. This means that patients who opt for SLN mapping over a lymphadenectomy aren't taking much more of a risk with their treatment choices.
What's Next for SLN Mapping
While SLN mapping is a safe and promising option for tracking cancerous endometrial cells, it is still considered a newer technology in the field of uterine cancer treatment. Several studies have shown that it is safe and effective at detecting cancer. Currently, large studies on SLN are underway to assess its superiority to full lymphadenectomy.
No matter what type of therapy your patient pursues at Moffitt, our multispecialty team will continually monitor her progress and adjust her treatment plan as necessary to ensure the best possible outcome and quality of life.
For the convenience of our patients and their referring physicians, all our gynecologic oncology services are available through a single program. Additionally, we prioritize short referral times to ensure that our patients can promptly receive the care they need and deserve.
If you'd like to refer a patient to a gynecologic oncologist at Moffitt Cancer Center, complete our online form or contact a physician liaison for assistance or support.
